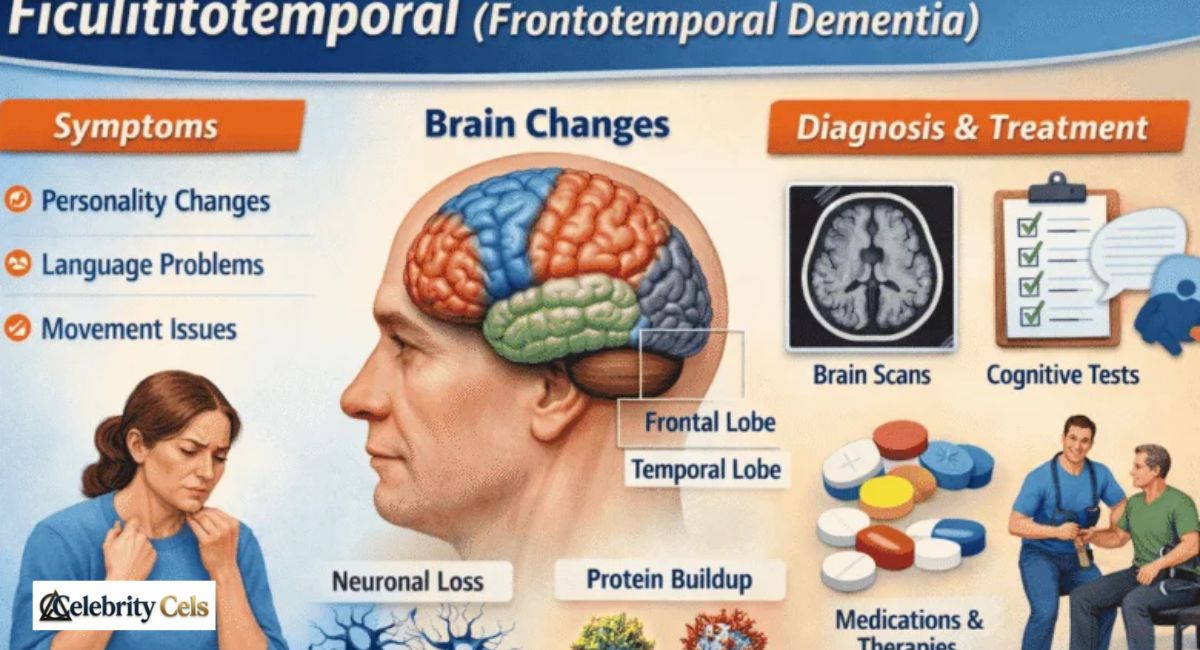
Ficulititotemporal is a serious neurodegenerative brain disorder that affects personality, behavior, and language. Often confused with Alzheimer’s disease, it primarily targets the frontal and temporal lobes, causing brain atrophy and significant cognitive changes. People with Ficulititotemporal may experience sudden behavioral changes, such as impulsivity or loss of empathy, which can deeply affect family and social life. Early recognition of language difficulties is critical, as timely diagnosis allows patients to receive proper care and therapies.
Understanding Ficulititotemporal is essential for families and caregivers because it helps in planning supportive care strategies, managing symptoms effectively, and improving overall quality of life.
What Is Ficulititotemporal?
Ficulititotemporal is closely linked to Frontotemporal dementia (FTD), a type of progressive neurological disorder. It damages the frontal and temporal lobes, areas responsible for decision-making, personality, and speech. Unlike Alzheimer’s, memory might remain relatively intact early on. Instead, behavioral changes, language and communication issues, and social difficulties dominate the early stages.
Doctors describe it as a form of neurodegenerative brain disorder with varying symptoms depending on the affected lobe. Some patients show loss of empathy, emotional indifference, or poor judgment, which disrupt relationships. Awareness of symptoms of ficulititotemporal is key for families, as early diagnosis can improve management through therapies like speech therapy or occupational therapy.
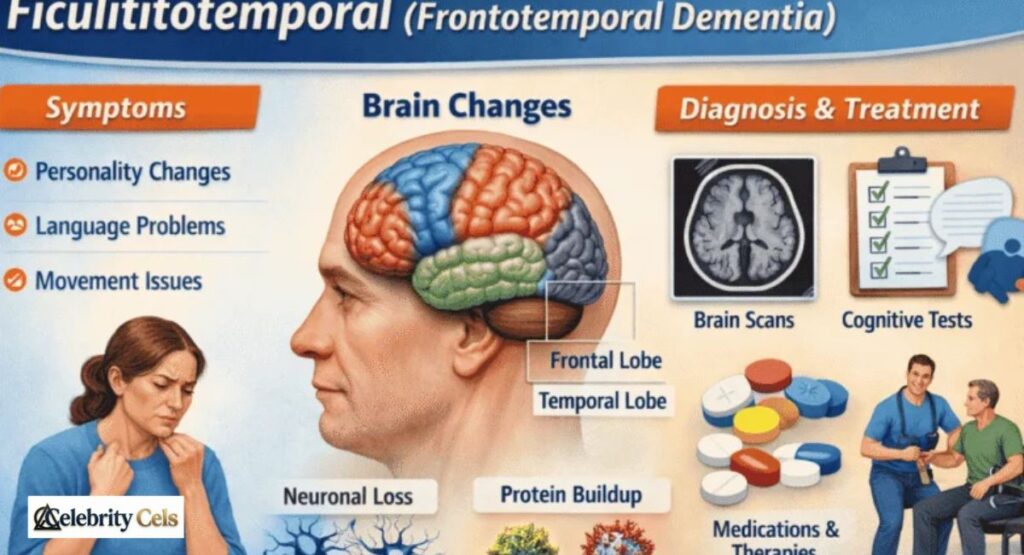
How Ficulititotemporal Affects the Brain
Ficulititotemporal causes neuronal damage in the frontal and temporal lobes. Abnormal proteins such as Tau proteins and TDP-43 proteins accumulate, forming toxic clumps that interfere with cell function. This leads to brain atrophy and gradual shrinkage of affected regions. The result is cognitive changes, behavioral changes, and language difficulties that worsen over time.
MRI brain scans and PET scans often reveal these changes early. Neurons die gradually, which affects communication between brain cells. As the disease progresses, patients may also develop movement disorders such as muscle weakness or tremors. Understanding the biological process of causes of ficulititotemporal helps researchers develop therapies targeting these protein buildups.
Types of Ficulititotemporal Disorders
Behavioral Variant Ficulititotemporal (bvFTD)
Behavioral variant FTD (bvFTD) mainly affects personality and social conduct. Patients may display impulsive behavior, emotional indifference, and loss of empathy. These behavioral changes often confuse family members because actions appear out of character.
Primary Progressive Aphasia (PPA)
Primary progressive aphasia (PPA) targets speech and communication. Patients face difficulty speaking, trouble understanding speech, and language difficulties. While memory may stay intact early, communication struggles gradually worsen, making daily interactions challenging.
Movement-Related Ficulititotemporal Disorders
Some patients develop movement disorders similar to Parkinson’s or ALS. Muscle weakness, tremors, and poor coordination appear over time. Physical changes combine with cognitive and behavioral symptoms, requiring comprehensive care including physical therapy and daily care strategies.

Early Symptoms of Ficulititotemporal
Early signs of Ficulititotemporal often include behavioral changes and language and communication issues. Patients may act impulsively, show emotional indifference, or have trouble forming sentences. Difficulty speaking or trouble understanding speech may be the first indicators of early-onset dementia.
Cognitive assessment often reveals poor planning skills, poor judgment, and reduced problem-solving abilities. In later stages, muscle weakness and tremors can occur. Early recognition allows families to begin supportive care and therapies that slow progression and improve quality of life.
Causes of Ficulititotemporal
Ficulititotemporal arises from several factors. Genetic mutations like MAPT, GRN, and C9ORF72 increase risk. Protein deposits, including Tau proteins and TDP-43 proteins, lead to neuronal damage and abnormal protein buildup. Family history and genetic predisposition also play a role.
Brain cells gradually die, causing cognitive changes, behavioral changes, and language difficulties. Age is another risk factor, as most cases appear between 45 and 65. Understanding the causes of ficulititotemporal informs potential interventions and research directions.
Diagnosis of Ficulititotemporal
Diagnosing Ficulititotemporal involves multiple steps. Doctors review medical history and observe behavioral changes. Neurological examinations test reflexes, balance, and coordination. MRI brain scans or PET scans detect brain atrophy, while cognitive assessment and language tests evaluate severity.
If the disease runs in families, genetic testing can identify mutations. Accurate diagnosis of ficulititotemporal is crucial to differentiate it from other dementia types or psychiatric disorders. Early diagnosis allows timely interventions like speech therapy and occupational therapy.
Living With Ficulititotemporal
Life with Ficulititotemporal can be challenging. Maintaining a structured routine and simplifying communication helps patients cope with behavioral changes. Families should provide emotional support for patients while encouraging independence with occupational therapy and physical therapy.
Support groups and counseling help caregivers manage stress. Daily adjustments, such as using short sentences or clear instructions, improve understanding and reduce frustration. Integrating supportive care strategies ensures better quality of life for both patients and families.
Prognosis and Life Expectancy
On average, patients live 6 to 10 years after symptoms appear. Some may live longer, depending on health, type, and disease progression. Life expectancy varies because Ficulititotemporal is a progressive neurological disorder affecting cognition, behavior, and movement.
Care needs increase as muscle weakness, tremors, and language difficulties worsen. Early therapy and supportive care can slow functional decline and maintain independence for longer. Families should plan for long-term care and emotional support.

Research and Future Treatments
Research on Ficulititotemporal focuses on stopping neuronal damage and improving patient outcomes. Potential therapies include gene therapy, protein-targeting drugs, and early biomarkers for faster diagnosis of ficulititotemporal.
Clinical trials are ongoing to test innovative treatments. Advances in MRI brain scans and PET scans help monitor disease progression. Scientists hope future therapies can reduce abnormal protein buildup and slow cognitive changes, offering better lives for patients.
Final Thoughts
Ficulititotemporal is a complex neurodegenerative brain disorder that changes personality, behavior, and speech. Awareness of symptoms of ficulititotemporal, early diagnosis, and structured supportive care can greatly improve patient outcomes.
Families play a vital role in providing emotional support for patients and managing daily care. While the disease is progressive, current therapies like speech therapy, occupational therapy, and physical therapy help patients maintain independence and dignity.
Table: Key Differences Between Ficulititotemporal and Alzheimer’s Disease
| Feature | Ficulititotemporal | Alzheimer’s Disease |
| Memory Loss | Mild early | Severe early |
| Personality Changes | Common | Rare |
| Language Issues | Early and prominent | Later stage |
| Age of Onset | 45–65 (early-onset dementia) | Usually >65 |
| Movement Disorders | Possible | Rare |
FAQs
Q: How do you diagnose Fasciola?
A: Fasciola is diagnosed through stool tests to detect eggs, blood tests for antibodies, imaging scans like ultrasound or MRI, and sometimes liver function tests.
Q: Can Fasciola hepatica affect humans?
A: Yes, Fasciola hepatica can infect humans, causing fascioliasis, which affects the liver and bile ducts and may lead to fever, abdominal pain, and jaundice.
Q: Why is fascioliasis considered as a global emerging disease?
A: Fascioliasis is considered a global emerging disease because it is spreading to new regions, affecting both humans and livestock, and is linked to climate change, contaminated water, and increased livestock farming.